Monday, July 27, 2009
Case of the Week 79
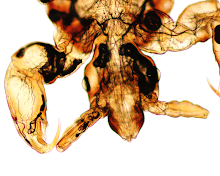
The following peripheral blood smear is from a 42 year old woman from Venezuela. Identification? (CLICK ON IMAGE TO ENLARGE)

Sunday, July 26, 2009
Answer to Case 79
Answer: Trypanosoma cruzi
It is important not to forget about these extracellular parasites when screening a blood smear for malaria parasites. This image shows the motile trypomastigotes of T. cruzi. Note that these organisms are approximately 2-3 RBCs in length, and contain a nucleus and kinetoplast (below, arrow). T. cruzi can be most readily distinguished from the trypomastigotes of Trypanosoma brucei by the size of the kinetoplast; the former is much larger and appears to bulge from the organism.

An interesting tidbit: Contrary to expected, the kinetoplast is at the posterior end of the organism, while the flagella is at the anterior end. The trypomastigotes move with their flagella at their front.
Thanks to the four folks who wrote in with the answer - all correct!
It is important not to forget about these extracellular parasites when screening a blood smear for malaria parasites. This image shows the motile trypomastigotes of T. cruzi. Note that these organisms are approximately 2-3 RBCs in length, and contain a nucleus and kinetoplast (below, arrow). T. cruzi can be most readily distinguished from the trypomastigotes of Trypanosoma brucei by the size of the kinetoplast; the former is much larger and appears to bulge from the organism.

An interesting tidbit: Contrary to expected, the kinetoplast is at the posterior end of the organism, while the flagella is at the anterior end. The trypomastigotes move with their flagella at their front.
Thanks to the four folks who wrote in with the answer - all correct!
Monday, July 20, 2009
Case of the Week 78
Sunday, July 19, 2009
Answer to Case 78
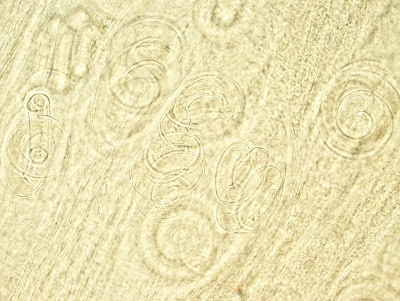
Identification: Trichinella spp. larvae
These are stage 1 larvae that were released from the female in the gut of the infected human, and then entered the blood stream and migrated to skeletal muscle. The type of preparation shown here is commonly called a "squash prep" since it is prepared by pressing or squashing a piece of muscle between 2 slides, or by using an instrument called a trichinelloscope. Note how the larvae are tightly coiled within the skeletal muscle fibers. There are different species of Trichinella that can infect humans and they are not distinguishable by morphology alone.
Congratulations to Salbrent and Sandhya who go the diagnosis correct.
These are stage 1 larvae that were released from the female in the gut of the infected human, and then entered the blood stream and migrated to skeletal muscle. The type of preparation shown here is commonly called a "squash prep" since it is prepared by pressing or squashing a piece of muscle between 2 slides, or by using an instrument called a trichinelloscope. Note how the larvae are tightly coiled within the skeletal muscle fibers. There are different species of Trichinella that can infect humans and they are not distinguishable by morphology alone.
Congratulations to Salbrent and Sandhya who go the diagnosis correct.
Monday, July 13, 2009
Case of the Week 77
The following organisms were found in a patient who presented with abdominal pain, bloody diarrhea, and a recent travel history to Mexico. They measure approximately 15 to 20 microns in greatest dimension. How should this be identified when using the stool ova and parasite examination alone? (CLICK ON IMAGES TO ENLARGE)




Answer to Case 77
The correct answer for this case is: Entamoeba histolytica/E. dispar
Note that I've listed 2 separate protozoan parasites, separated by a slash. It is not possible to distinguish these organisms by morphologic grounds unless you see ingested RBCs in the trophozoites which are strongly suggestive of E. histolytica. Since there are none present in these images, this specimen should be reported out as E. histolytic/E. dispar, with a recommmendation for correlation with clinical presentation and additional lab testing such as serology, stool antigen testing, and/or stool PCR. Clinically, E. histolytica is a known pathogen, and can cause bloody diarrhea and disseminated disease. E. dispar, on the other hand, is NOT thought to cause disease. Since E. dispar is much more prevalent than E. histolytic, it is important to perform additional testing that will allow definitive speciation.
Congratulations to "Rabies Testing Lab" who got all of the caveats correct in this case!
On a stool preparation, the diagnosis of E. histolytica/E. dispar is made on the classic appearance of the cyst and trophozoite forms seen here, paying particular attention to the "ring and dot" nuclear chromatin pattern of Entamoeba spp. Size is also very important for making an accurate diagnosis, since other Entamoeba can look very similar, but differ in size.
Note that I've listed 2 separate protozoan parasites, separated by a slash. It is not possible to distinguish these organisms by morphologic grounds unless you see ingested RBCs in the trophozoites which are strongly suggestive of E. histolytica. Since there are none present in these images, this specimen should be reported out as E. histolytic/E. dispar, with a recommmendation for correlation with clinical presentation and additional lab testing such as serology, stool antigen testing, and/or stool PCR. Clinically, E. histolytica is a known pathogen, and can cause bloody diarrhea and disseminated disease. E. dispar, on the other hand, is NOT thought to cause disease. Since E. dispar is much more prevalent than E. histolytic, it is important to perform additional testing that will allow definitive speciation.
Congratulations to "Rabies Testing Lab" who got all of the caveats correct in this case!
On a stool preparation, the diagnosis of E. histolytica/E. dispar is made on the classic appearance of the cyst and trophozoite forms seen here, paying particular attention to the "ring and dot" nuclear chromatin pattern of Entamoeba spp. Size is also very important for making an accurate diagnosis, since other Entamoeba can look very similar, but differ in size.
Monday, July 6, 2009
Case of the Week 76
I think it is very fitting that we have Case 76 right after our July 4th celebration.
The following sections of placenta are from a still-borne infant with severe growth retardation. On gross examination, the placenta was smaller than normal and had several infarcts. Microscopic examination showed erythrocytes with brown pigment and inclusions, as well as chronic villitis, synctial knotting, and pigment in trophoblastS and WBCs. Diagnosis? For the hematopathologists in the audience, there is another diagnosis present as well...
(CLICK ON IMAGES TO ENLARGE)




The following sections of placenta are from a still-borne infant with severe growth retardation. On gross examination, the placenta was smaller than normal and had several infarcts. Microscopic examination showed erythrocytes with brown pigment and inclusions, as well as chronic villitis, synctial knotting, and pigment in trophoblastS and WBCs. Diagnosis? For the hematopathologists in the audience, there is another diagnosis present as well...
(CLICK ON IMAGES TO ENLARGE)




Sunday, July 5, 2009
Answer to Case 76
Answer: Placental malaria. Plasmodium falciparun would be the most likely suspect. The diagnosis is made by identification of malaria pigment and inclusions within RBCs and macrophages (see image below). Note that some of the RBCs display prominent sickling. Interestingly, the sickled cells and malaria parasites are all within the maternal circulation in this case.

One of the viewers asked if homozygous sickle cell (Sickle cell disease) wasn't completely protective against malaria. Studies have shown that both sickle cell disease and trait (heterozygous expression)offer a protective benefit against malaria, but it is not absolute protection.
For example, in a large cohort study of children in Kenya, sickle cell trait was 50% protective against mild clinical malaria, 75% protective against hospitalization for malaria, and 90% protective against severe or complicated malaria.
Reference:
Williams TN, Mwangi TW, Wambua S, et al. Sickle cell trait and the risk of Plasmodium falciparum malaria and other childhood diseases. J Infect Dis. 2005;192:178–186.
Thanks for writing in with your comments and questions!

One of the viewers asked if homozygous sickle cell (Sickle cell disease) wasn't completely protective against malaria. Studies have shown that both sickle cell disease and trait (heterozygous expression)offer a protective benefit against malaria, but it is not absolute protection.
For example, in a large cohort study of children in Kenya, sickle cell trait was 50% protective against mild clinical malaria, 75% protective against hospitalization for malaria, and 90% protective against severe or complicated malaria.
Reference:
Williams TN, Mwangi TW, Wambua S, et al. Sickle cell trait and the risk of Plasmodium falciparum malaria and other childhood diseases. J Infect Dis. 2005;192:178–186.
Thanks for writing in with your comments and questions!
Subscribe to:
Posts (Atom)